How to Support Students with Diabetes
Written by: Ginger Vieira
9 minute read
March 2, 2026
A student with type 1 diabetes (T1D) may need support at school from teachers or fellow classmates because of low blood sugar. When this happens, it’s important to be aware of how you can step up and why it matters!
First, what is type 1 diabetes?
Type 1 diabetes is an autoimmune disease in which a person’s own immune system attacks and destroys the cells in the body that produce insulin. Anyone can be diagnosed with T1D at any age—not just kiddos.
Without enough insulin, the body cannot use the sugar—aka glucose—in the bloodstream for energy. When T1D is left undiagnosed or untreated, blood sugar levels can quickly become life-threatening.
For people without diabetes, blood sugar levels are maintained by a steady balance of the hormones insulin and glucagon. This natural bodily process keeps you safe and healthy all day and all night.
Whereas a person with insulin-dependent diabetes (all people with type 1 and some people with type 2 needs to do the work themselves!
What’s it like to have type 1 diabetes?
People with T1D need to take insulin every single day through multiple injections (MDI) with a syringe or pen, inhaled insulin, or use an insulin pump or pod attached to their body. This includes children and teens
Type 1 diabetes never lets up. People with T1D or parents of children with T1D have to try to match their insulin doses to the food they eat and to other factors that can raise their blood sugar, such as exercise and stress.
Perhaps one of the biggest challenges and scary parts of the gig is low blood sugar, aka hypoglycemia. This happens when someone with T1D has too much insulin on board (IOB), which means that the insulin that is still working in your body from a past dose.
What is low blood sugar?
Low blood sugar is a blood sugar level at or below 70 mg/dL/3.9 mmol/L. Thebody—and primarily the brain—cannot function without enough glucose. The brain relies on a second-by-second delivery of glucose.
Low blood sugars can happen when:
- Too much insulin is taken
- Too much insulin is in the bloodstream during physical activity
- Too much background/basal/long-acting insulin is on board
- Meals are skipped or not eating enough
Pay close attention during recess and right after meals, as these are the times when children with T1D are most at risk of low blood sugar emergencies.
Common symptoms of low blood sugar include:
- Blurred vision
- Cold sweats
- Confusion
- Cool, pale skin
- Difficulty concentrating
- Drowsiness
- Excessive hunger
- Feeling anxious
- Fast heartbeat
- Headache
- Nausea
- Nervousness
- Nightmares
- Restless sleep
- Shakiness
- Slurred speech
- Sudden changes in behavior—either aggressive or goofy (in adults, they might seem drunk without drinking)
- Unusual tiredness or weakness
If your classmate or student shows signs of low blood sugar, you can suggest they may be low and encourage them to check their blood sugar with their blood glucose meter (BGM) or continuous glucose monitor (CGM).
It might feel awkward, but it’s worth it if it saves their life.
You should also ask an adult nearby for help. Follow the child or teen’s low blood sugar preparedness plan, if they have one, which may include calling the school nurse and/or their parents.

Shot of a young girl sleeping at her desk in a classroom
How to help treat low blood sugar at school
When a student with T1D is experiencing a standard low blood sugar, you can help them treat it by getting fast-acting carbohydrates to eat or drink. School-aged children or teens should have a stash of fast-acting carbohydrates in their backpack or desk. You can also ask your school administrator to provide snacks for you to keep in your classroom. –
Fast-acting carbohydrates are foods or drinks that have no dietary fat or protein, which makes it easier for the digestive system to break down into glucose and raise blood sugar levels.
Most low blood sugar episodes require about 15 grams of fast-acting carbohydrate to return to a safe level about 15 minutes after consumption. This is a general guideline that sometimes varies by individual. If you’re unsure what a child or teen with T1D’s exact plan is, this is a safe place to start.
Examples of fast-acting carbohydrates:
- 4 oz of fruit juice
- A handful of jelly beans
- 3 or 4 glucose tabs
- 1 pack of gummies or fruit snacks
After the student has eaten 15 grams of fasting acting carbohydrates, wait 15 minutes, and recheck their blood sugar. If they are still below 70 mg/dL/3.9 mmol/L, they’ll need to eat another 15g of fast-acting carbohydrates. If they continue to have low blood sugar after that, they’re likely experiencing a more severe low blood sugar, and you should move to take next steps.
It’s important to note that a student experiencing low blood sugar should never be left alone or asked to walk to the nurses office for treatment.
What is severe low blood sugar?
When a student with T1D’s blood sugar level drops below 3.1 mmol/L (55 mg/dL), symptoms of severe low blood sugar can occur, including:
- Unable to eat or drink
- Seizures and convulsions
- Loss of consciousness
- Coma
In some cases, untreated severe low blood sugar episodes can be life-threatening. If your classmate or student is experiencing symptoms of severe low blood sugar and is not alert or awake enough to eat or drink their low blood sugar treatment, it’s time to use emergency glucagon.
What is an emergency glucagon?
While most people are familiar with the EpiPen and its life-saving role during severe allergic reactions (like those from a bee sting or peanuts), emergency glucagon is still largely unknown. This needs to change!
Glucagon is a hormone produced by your pancreas that signals your liver to release stored sugar (glycogen), helping prevent low blood sugar in people without diabetes.
Emergency glucagon is used to treat severe low blood sugar.
While people with diabetes do produce glucagon, they cannot always produce the amount needed during severe low blood sugar events. And that is why emergency glucagon is so important.
Emergency glucagon should be used when:
- Food or drink is not correcting low blood sugar
- Someone is unable to eat or drink
- Someone is seizing or convulsing
- Someone is unconscious
- Someone is unresponsive
Make sure you know where your classmate or student keeps their emergency glucagon. Talk with the child or teen and their parents about this as soon as you learn they have T1D, just to be safe.
Hopefully, you never have to use it, but it’s good to be aware in case you do.
Types of emergency glucagon
There are many easy-to-use emergency glucagon treatment products available today, including:
- Nasal glucagon—Baqsimi®: This is an emergency glucagon that’s administered through your nose.
- Glucagon pen—Gvoke HypoPen®: This is a premixed glucagon injection that you press against your thigh. The auto-inject device makes it quick and easy to use. It is also available in a prefilled syringe (PFS).
- Glucagon Prefilled Syringe—Gvoke Kit®: This is a premixed glucagon in a vial that comes with a syringe, allowing you to draw up the dose manually and inject it directly into your thigh.
- Glucagon pen—Zegalogue®: Also a premixed glucagon, available as an easy-to-use auto-inject device. It is also available in a prefilled syringe (PFS).
How to use emergency glucagon on someone with T1D
Time is critical during a severe low blood sugar episode. Be proactive and learn what to do before a severe low blood sugar event occurs.
If you ever need to use glucagon on your student or classmate, here’s what you should know:
- Make sure they are physically safe if unconscious or seizing: If someone with T1D starts to experience a seizure, for example, when they are standing up or walking—yes, it’s possible—it’s important to carefully move them to a safe position and location. Before or during a seizure, do your best to make sure they are physically safe from other hazards, falls or even nearby cars if the seizure occurs on the side of the road.
- Call 911: As soon as you notice someone is experiencing severe low blood sugar, call 911.
- Locate their emergency glucagon: The most important thing someone with diabetes can do is teach their friends, family and coworkers about the location of their emergency glucagon. With kids, this is often the parents’ responsibility. It’s important to ask and know the location of their emergency glucagon treatment. Encourage them to keep it with them at all times.
Follow the directions on the glucagon treatment (glucagon is prescription-only and will be specific to each student):
- Nasal glucagon: Place the person on their side. Remove the cap. Insert the tip gently into their nostril and press the plunger end firmly until the green line disappears.
- Auto-inject pen: Place the person on their side. Remove the red (Gvoke) or grey (Zegalogue) cap. Press the yellow end of the pen against their upper arm, stomach, or thigh and hold for five seconds (Gvoke) or 10 seconds (Zegalogue).
- Pre-filled syringe: Place the person on their side. Remove the syringe cap. Pinch the skin and insert the needle at a 90‑degree angle. Push the plunger down as far as it will go. Inject the glucagon into their upper arm, stomach, or thigh.
Look out for severe low blood sugar side effects
Stay with them as they recover until emergency crews arrive. When someone with T1D regains consciousness after receiving emergency glucagon, they can experience symptoms including vomiting, confusion and panic. Keep them on their side to ensure they are safe during any of these side effects.
Talk to your students or classmates who have diabetes. Let them know you are willing to learn how to help them during low blood sugars!
Are you passionate about spreading awareness of the signs and symptoms of type 1 diabetes? Join our #SeeTheSigns movement. Share a simple message that makes a real impact!
This educational content on Back to School is made possible with support from Lilly Diabetes (Baqsimi), an active partner of Beyond Type 1 at the time of publication. Editorial control rests solely on Beyond Type 1.
Related Resources

It’s fair to assume that a 911 call about severe low blood sugar (hypoglycemia) will...
Read more
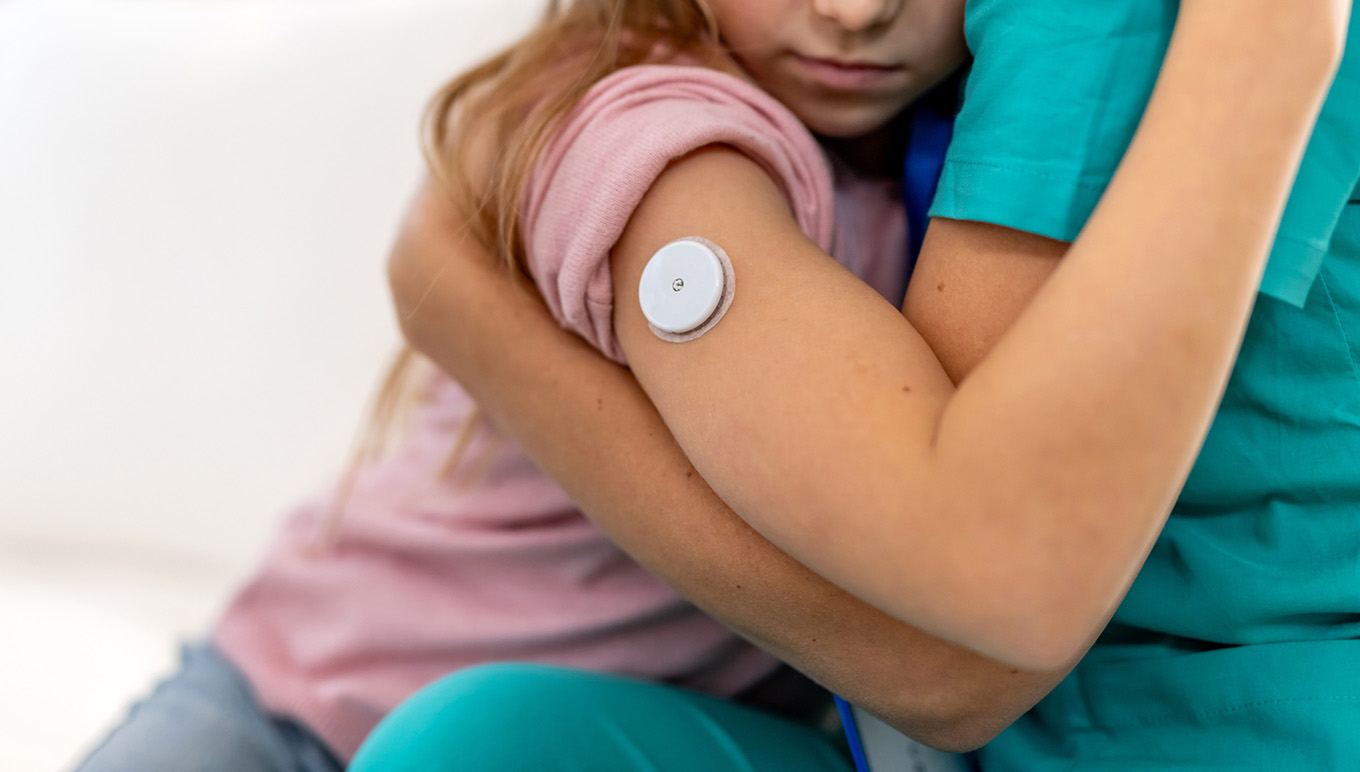
Low blood sugar can make people with diabetes (PWD) feel exhausted, frustrated and scared. Sometimes,...
Read more

Sensitive Topic Warning: For some people, eating a lot of food all at once when...
Read more


