My 10-Year Old Can Save My Life
Written by: Rebecca Redmond
4 minute read
May 22, 2020
Editor’s Note: This article was part of Beyond Type 1’s focus on hypoglycemia and severe hypoglycemia during our Let’s Talk Lows campaign. We looked at causes, symptoms, fears and treatment options. Follow along using the hashtag #LetsTalkLows and share your hypoglycemia experiences with the community.
Anyone familiar with type 1 diabetes has heard the term hypo or low when discussing blood glucose levels. And, whether you are someone with type 1 diabetes (T1D) or someone who cares for a T1D, chances are you have been privy to the dreaded beast that is hypoglycemia.
Hypo Hot Mess
When I was diagnosed in 1999, I was already familiar with type 1 diabetes and insulin. You see, I have a deep family connection to it all. Sir Frederick Banting is my cousin. And while I was long familiar with diabetes, the finer details were unknown until I was living with it myself.
And those finer details include hypos.
During my post-diagnosis education, it was loosely suggested that I fill the prescription for a glucagon kit with no real explanation about what it was or when to use it. At that time, it had to be stored in the fridge, was terribly expensive (I had no coverage), and so, not a priority because I had never experienced a “bad low.”
Yet.
Bad Night
 No two days with diabetes are ever the same. You can literally do the exact same thing in the exact same way and have a totally different result the second time.
No two days with diabetes are ever the same. You can literally do the exact same thing in the exact same way and have a totally different result the second time.
Living with T1D means you are likely going to be faced with a severe hypo episode at some point. I had experienced a handful of baddies in my time, but nothing like the night the ambulance came to our home.
I wish I could remember exactly what happened. It would certainly be helpful for both the telling of this story and prevention. What I do remember is how I felt. I can physically remember what my body went through that evening.
It happened more than a decade ago. And we did not have glucagon in the house.
I cannot recall the moments leading up to it, my first memory of that night is being on the floor of our lower level washroom. I remember my skin being on fire. So prickly it stung. From the inside. I was on the floor crying in pain, attempting to cool off, but also going in and out of consciousness.
My husband had juice and was pricking my finger performing yet another blood glucose test. I do not know how many pricks he did before he called the ambulance. I know that every single one of them came back LO. Even though I cannot clearly remember the movements of that evening, I will never forget the look on his face.
My next memory occurs in our upstairs living room. I am in a chair and speaking with a paramedic who reminds me of my brother. I remember them saying they would stay until my blood sugars stabilized above 4.5 mmol/L (80mg/dL).
And I remember them strongly suggesting we get a prescription for glucagon and fill it.
Life Saving Costs
Before I became pregnant, we never had glucagon in the house. It was difficult to justify spending the money on something that sat in the fridge until it expired.
Even that scary episode did not shake me enough to spend the money (that we did not have).
But pregnancy/motherhood changed me, in more ways than weight gain and stretch marks. Suddenly my body was a vessel responsible for another living being. It marked the start of a serious change in my management. And that included bringing glucagon (back) into our home.
After our son was born, I would always carry a kit with me, in my purse. We even held on to an expired one and left it in the fridge at home.
Going forward we always made sure we had squirreled away enough to cover the cost of replacing the expired kit. A few years later, we learned the shelf life/storage guidelines had changed. And we were able to get some coverage.
Now there was no excuse not to have it.
Life Saving Reluctance
From a young age, we have educated our son about my type 1 diabetes. By the time he was 18 months old, he could test my blood sugars on his own. He knew the signs of lows. And when he was 4 years old, we taught him how to inject glucagon.
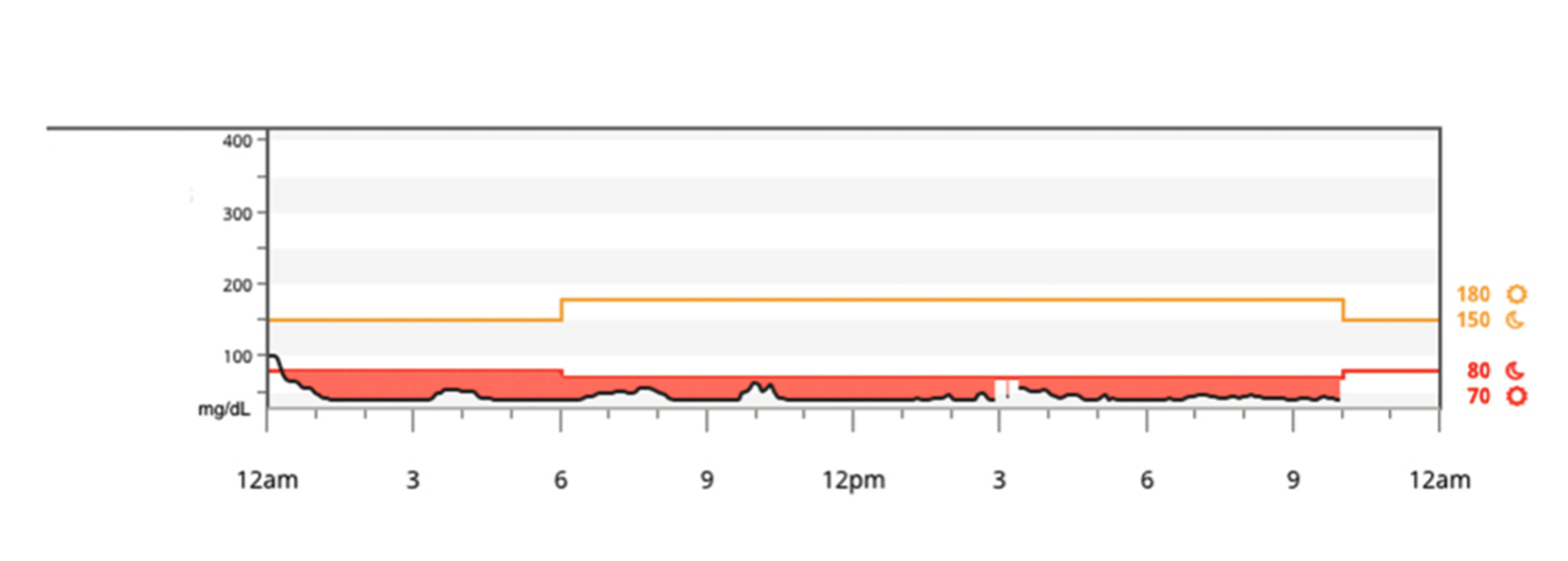
Around that same time, I was offered a continuous glucose monitor (CGM) for a week. It was an incredible experience. And, sadly, one we could not afford to continue. Without being able to see how my blood sugars are trending, management remained reactive.
However, the idea of injecting the glucagon was daunting. For both my husband and my son.
My husband always said it is impossible to keep anything straight when dealing with a loved one experiencing severe hypoglycemia. He references the bad night and says even if we had a glucagon in the house, he is not confident he could have correctly remembered the many steps involved in its administration. And he remained leery of being able to mix/administer with confidence.
My son had expressed the same concerns. Along with the fact that he is not a fan of needles and, “having to mix the glucagon and stab Mommy,” is something he finds incredibly frightening. All that puts a tremendous amount of pressure on us all. Especially as I work from home and we homeschool.
That means my son and I are alone at home together. A lot of the time.
And a bad low is bound to happen.
Diversifying Dispensing
Advancements in medicine come in many shapes, and recently in the form of new kinds of glucagon, like Baqsimi. It is glucagon that does not require the dose be administered through injection. Instead, it is a nasal powder that does not need to be inhaled.
I first became aware of nasal glucagon in the late spring of 2019, and immediately set to work finding out when it would be available in Canada. When I shared the news with my family, they were over the moon. We made it our mission to add Baqsimi to my T1D toolbox.
In December 2019, our pharmacy called to inform me they would be ordering my glucagon, but it would take a week to come in, and let me know when it was available. I put the phone down confused.
I had two kits in the house.
A week later my husband arrived home with a box: Baqsimi. I had completely forgotten asking my endocrinologist for a prescription months earlier! Thankfully, our benefits helped cover the cost.
That day, we all sat down and learned how to properly administer nasal glucagon.
The look of relief on the faces of my husband and son were priceless. Not only were there significantly less steps (2 vs 10-ish), administering the glucagon was easy. Plus, no needles!
Less steps and no fear/hesitation mean a quicker solution, according to my husband. And an easy solution makes a scary situation less so, according to my son.
He says, “that makes it easier to help Mommy and not be afraid.”
And that kind of peace of mind is invaluable.
Educational content related to severe hypoglycemia is made possible with support from Lilly Diabetes (BAQSIMI), an active partner of Beyond Type 1 at the time of publication. Editorial control rests solely on Beyond Type 1.

Author
Rebecca Redmond
Rebecca Redmond is a passionate creative type who has been writing and drawing pictures for as long as she can remember. Most recently, she has expanded to blogging and public speaking, sharing her experiences living with type 1 diabetes and mental illness as she advocates on a global scale in an intimate setting. She continues to explore her artistic passions currently with a type 1 diabetes (T1D) theme. Instagram - @rebaredmond (personal) @deadpancreasanxiety (blog) or #bangtingst1dcousin Facebook – Rebecca Redmond or Dead Pancreas Anxiety Twitter - @RebaRedmond
Related Resources
My friend always refers to them as the “come at me bro” arms, but more...
Read more

Editor’s Note: This week, Beyond Type 1 will be focusing on hypoglycemia and severe hypoglycemia...
Read more

Editor’s Note: This week, Beyond Type 1 will be focusing on hypoglycemia and severe hypoglycemia...
Read more


