Lost In Translation: Diabetes Care In A Language That Isn’t Yours
Written by: Katherine Gilyard
6 minute read
April 15, 2026
If you’ve ever left a diabetes appointment more confused than when you arrived, it’s not you—it’s the system.
When we talk about language barriers in diabetes care, we usually mean the literal kind: you speak one language, your provider speaks another. That’s real.
But there are at least five “languages” that can lock you out of your own care and most of them have nothing to do with what tongue you speak. These languages are jargon, insurance, clinical data and cultural assumptions. And they stack on top of each other.
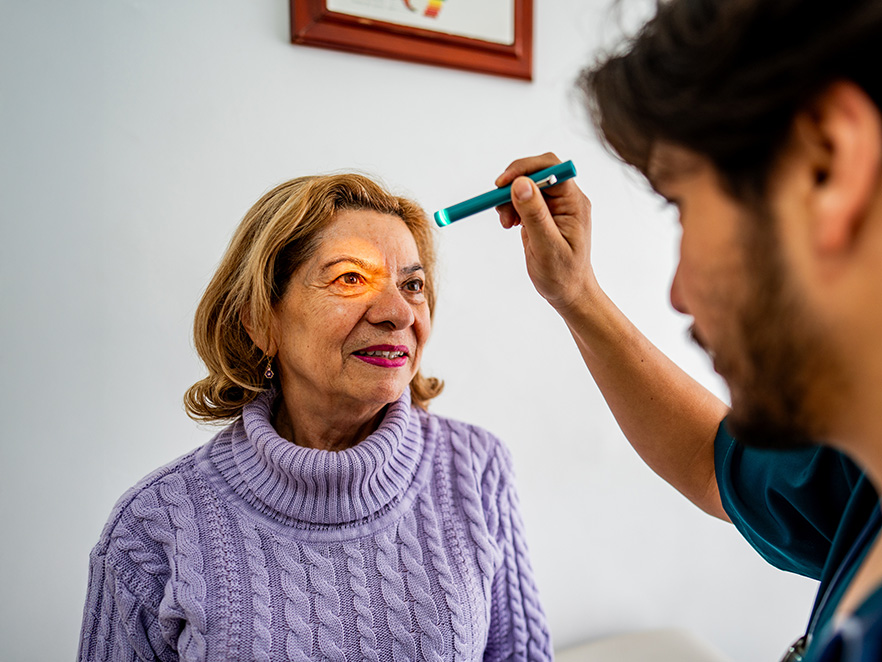
What happens when you and your healthcare provider don’t share a language?
A UCSF and Kaiser Permanente study found that among Latinx people with limited English, those with doctors that didn’t speak Spanish were nearly twice as likely to have poor blood sugar control—even when interpreters were available.
Under Title VI of the Civil Rights Act, healthcare facilities that receive federal funding are legally required to offer you language access services. But what’s legally required and what actually happens in a rushed appointment are often two different things.
When interpreters aren’t available, many people lean on family members—sometimes children—to translate conversations about insulin doses and lab results. Instructions like “take with food” or “as needed” may get lost or flattened. In those cases, the nuance that diabetes management depends on disappears.
What about medical jargon?
You don’t have to be a non-English speaker to feel lost when your healthcare provider uses a lot of medical terms.
A1C, basal/bolus, time in range, contraindicated, diabetic ketoacidosis (DKA)—these terms can get thrown at you without explanation and you’re expected to keep up.
Research shows that even people who’ve lived with diabetes for years can sometimes struggle with all of the terminology their providers use every day. According to a national literacy assessment, 36% of U.S. adults have basic or below-basic health literacy.
The shame of nodding along when you don’t understand is real. And often healthcare providers don’t realize that they’re speaking a language you don’t know. The CDC has developed a plain-language glossary for diabetes education, but healthcare provider training in clear communication remains inconsistent.
What about insurance language?
Prior authorization. Formulary. Step therapy. Medical necessity. The language of insurance isn’t just confusing, it can feel designed to confuse.
When your claim for a continuous glucose monitor (CGM) comes back “denied,” it reads like a final answer. But “denied” doesn’t always mean “no.” It often means that your next step is to “appeal.” The problem? Nobody tells you that.
Navigating insurance requires its own literacy and most people with diabetes are left to figure it out alone, often while managing the very condition that makes the paperwork so urgent.
What about the numbers?
“Your A1C should be under 7.” You’ve probably heard some version of this from your healthcare provider.
But have they actually explained what that number actually means—or whether that target is realistic for your life right now?
Clinical targets, risk percentages and study results are often presented to people with diabetes as neutral facts. But in practice, they can be used to judge. A number without context becomes a grade, not a tool. When targets get handed down without a conversation about what’s actually going on in your life, they become another language you’re expected to speak fluently without anyone teaching you.
What about the assumptions your provider makes about you?
Maybe the most insidious language barrier isn’t about words at all. It’s the set of assumptions a healthcare provider may bring into the room about what you can and can’t handle—based on your race, your insurance card or how they read your socioeconomic status.
Research from the T1D Exchange found that healthcare provider implicit bias shapes who gets recommended for diabetes technology.
Providers were more likely to recommend insulin pumps and CGMs for people with private insurance and English-sounding names. A 2024 review in Clinical Diabetes found that Black people and those on Medicaid or Medicare were more likely to be labeled “nonadherent”—which means not following the medical recommendations from your healthcare provider—even when their A1C levels matched those of white, privately insured people.
And once that label sticks, the conversation shifts from support to suspicion.
But bias doesn’t only show up in technology access. It shows up in diet advice that assumes you have access to certain foods, a stable schedule and money to spend. It shows up in “lifestyle change” recommendations that ignore shift work, caregiving, food deserts and housing instability. Or it may show up in the unspoken assumption that you have time, money and support, or that you don’t, and therefore aren’t worth the investment. In any of these situations, the healthcare provider is responding to a story in their head, not the actual person in front of them.
So what can you do about it?
These barriers stack. If you’re navigating diabetes in a second language, you’re also more likely to face jargon you can’t decode, insurance language nobody explained and provider assumptions shaped by bias. But naming the problem is the first step.
Organizations like the American Diabetes Association have pushed for person-centered, strengths-based communication in diabetes care—language that puts you first, not your numbers. Beyond Type 1’s Beyond Barriers program is working to bring resources and education directly into underserved communities, meeting people where they are instead of expecting them to navigate a system that wasn’t built with them in mind.
- Advocate for yourself. Ask your healthcare provider to explain terms in plain language. If something doesn’t make sense, say so
- Ask about technology and treatment options even if your healthcare provider doesn’t bring them up
- Challenge an insurance denial—it’s not always final.
And remember: if your care feels like it’s happening in a language you don’t speak—it might be. That’s not your fault. The system owes you better.
Want to learn more about health equity in diabetes care? Explore Beyond Type 1’s Beyond Barriers program and find organizations serving underserved communities in our resource directory.

Author
Katherine Gilyard
Beyond Type 1 is the largest diabetes org online, funding advocacy, education and cure research. Find industry news, inspirational stories and practical help. Join the 1M+ strong community and discover what it means to #LiveBeyond a diabetes diagnosis.
Related Resources

In life with diabetes, freebies are pretty much unheard of. The cost of diabetes is...
Read more

A new routine can feel like a reset, whether it’s a new year or a...
Read more

Diabetes is physically, mentally and emotionally taxing. There are no days off and few breaks....
Read more

