Surviving a High-Risk Pregnancy with Type 1 Diabetes
Written by: Dalila Brent
6 minute read
April 15, 2026
Pregnancy is never a one-size-fits-all experience, especially when you’re navigating it alongside a chronic condition like type 1 diabetes. What often begins as a moment of excitement can quickly shift into a complex, high-risk journey. For Lexie Peterson—known to many on social media as @thedivabetic—that reality set in as her pregnancy unfolded with a series of unexpected complications that had little to do with diabetes, but everything to do with the unpredictability of maternal health.
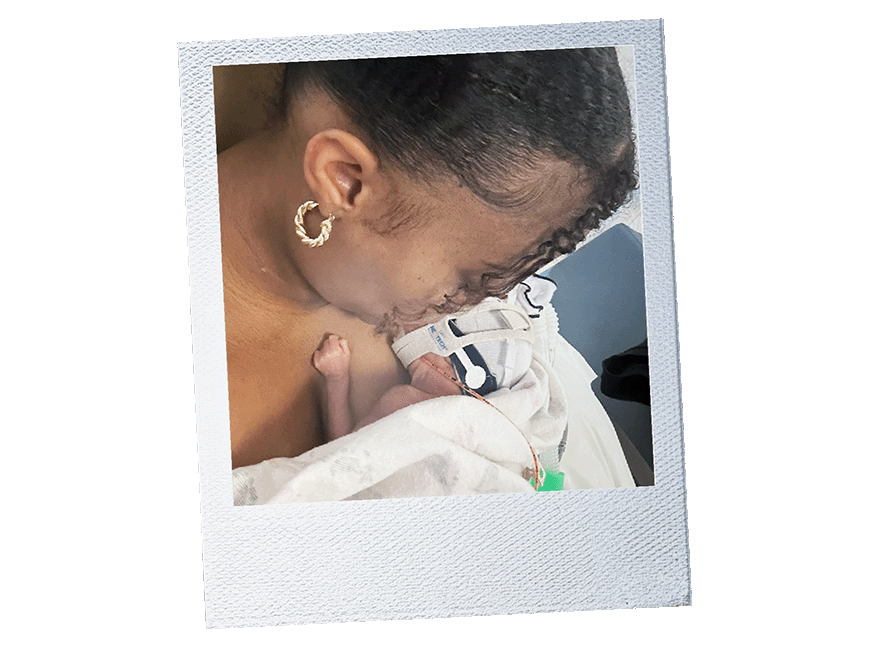
In recognition of Black Maternal Health Week (April 11–17), Peterson is sharing her story, from bed rest and emergency surgery to her daughter’s 65-day stay in the neonatal intensive care unit (NICU), to shed light on the importance of self-advocacy, trusted care teams and the urgent need for better outcomes for those navigating pregnancy—especially Black women.
*Responses have been edited for brevity and clarity
Expecting the unexpected
I found out I was pregnant the day after, I got back from a diabetes conference. I was in Orlando for Friends for Life, and the whole time I was there I felt more tired than usual. Anytime I tried to sip wine or anything, my stomach would tighten up, so I just stopped trying, thank God. When I got home, I took a pregnancy test because my period was late—but I also have PCOS, so my periods are really irregular and I didn’t think much of it. And then, lo and behold, I was pregnant. It was a shock—I was nervous, excited, just a mix of everything, especially since I had just turned 30.

At my 12-week appointment, during my first ultrasound, my doctor told me I’d need to see a maternal-fetal medicine specialist because my OB-GYN wasn’t comfortable managing my diabetes during pregnancy. At my 20-week appointment, we found out I was even higher risk than I thought because I had a very short cervix. I was put on bed rest and started working from home, and about a week later there was basically nothing left, so they scheduled me for a cerclage procedure—stitching my cervix shut to try to keep it from opening further. The goal was to make it to at least 22 weeks, ideally 24.
But I ended up delivering at 27 weeks and one day. The day before, I thought I was having Braxton Hicks, but nurses were split on whether I should go in until a doctor friend told me to just go. When I got there, I was having real contractions, and they tried medication to slow things down and planned to keep me in the hospital on bed rest to get me closer to 28 weeks, but baby girl wasn’t waiting. My white blood cell count was high and they couldn’t confirm if there was an infection, so they decided on a C-section the next day—still planned, not yet an emergency. That night, she also flipped to breech, and the next morning I somehow got what was assumed to be an air embolism, which turned it into an emergency C-section. I don’t remember much because it happened so fast—I turned blue and they had to act immediately—but they saved both of us. My daughter was okay, but I was in the ICU for about 24 hours with a collapsed lung and my kidneys not functioning properly. As a diabetic, hearing that was terrifying because you immediately think dialysis, but thankfully everything eventually recovered.
Baby narratives, reframed
Before I got pregnant, I had always been told by different endocrinologists that my A1C should be between a 6 and 6.5, some even said below a 6, which I don’t even know how you achieve. When I conceived, mine was around 7.2 or 7.3, so I probably would have tried to get it lower if I had known. But as soon as I found out I was pregnant, I had tunnel vision about lowering my A1C because I thought all these bad things would happen if it wasn’t at a certain number. And I’m not saying you should just have a crazy A1C during pregnancy, but perfection is impossible. I was also under the impression I’d need to be induced or have a C-section because people with type 1 diabetes are told they tend to have very big babies—even if blood sugars are controlled. But when my baby was born, even though she was premature, she was still low birth weight for her gestational age. Based on how things were going with my diabetes management, she probably would have been a normal, healthy weight.
Fuel over fear
I was meal prepping religiously at the beginning of my pregnancy because my insulin resistance was high. I needed more insulin than usual to keep my blood sugar steady. But I didn’t realize at the time that what I was doing wasn’t exactly right. I was eating as low carb as possible, lots of protein, being really strategic about when and how much I ate, and walking after almost every meal. I just thought that was what I was supposed to do, but the issue is you actually need calories and carbs to help fuel your baby. Once I met with my endocrinologist, she explained that and helped correct me, and I also met with a registered dietitian who suggested meals that were lower on the glycemic index—so they wouldn’t spike my blood sugar as quickly—but still had the carbs and calories I needed. It was more about balance than restriction.
Trust your body, and instincts
Before making the decision to have a baby you really have to be in tune with your body—know yourself and know when something feels off—and have a solid understanding of your diabetes management. I was comfortable making changes on my own and then looping my endocrinologist in after, like, “Hey, I adjusted my insulin this week,” but I’ve lived with diabetes for 20 years, so I felt confident doing that. There were still moments that scared me, especially when my blood sugar would drop really fast—you can’t always prepare for that, and you don’t expect it. But that’s true with anything. If you want a baby or a family, you can’t let fear hold you back—you just prepare the best you can and make sure you have a strong support system, especially other women with type 1 who’ve been through it.
Black maternal health and the need for better care
Everybody that looks like us isn’t necessarily for us. I’ve had really bad experiences with Black doctors, not all of them, but enough to know I’m very intentional about who I choose. I think it’s important to get to know your doctor first; you can actually sit down and interview them before you establish care. I read reviews, I pay attention to what other patients are saying, and I’m quick to fire a doctor if something feels off because I don’t play about my health, especially now that I have a baby. So I really do my due diligence in finding who’s going to care for me, and I don’t base that decision solely on skin color. And I’ll say this too, I don’t think what happened to me was because I’m a Black woman. I hope not, but I have seen recently—especially on social media—multiple instances of Black women experiencing traumatic care during pregnancy. I feel like in a lot of those situations, those women were treated like they were just numbers. And I wish, first, that bad things wouldn’t happen in general, but also that when they do, people try to make it right—especially if it wasn’t intentional. But I also wish the intentional things wouldn’t happen. We should be treated just like everybody else. Why is our maternal mortality rate so much higher than our counterparts who are not women of color?
Advancing T1D pregnancy care
Are you currently pregnant (or planning to be) and living with type 1 diabetes? The Jaeb Center for Health Research is enrolling participants for “T1D Pregnancy & Me,” an observational study exploring how tools like continuous glucose monitors (CGMs) and automated insulin delivery (AID) systems support diabetes management during pregnancy. The goal is to better understand how these technologies work in real life, and where they fall short, so healthcare providers can better manage diabetes during pregnancy and improve outcomes for both mothers and babies.
We know Type 1 diabetes and pregnancy can feel overwhelming, but you don’t have to navigate it alone. Join our community to share your story and get your questions answered.
Related Resources

Parents of children and teens living with type 1 and type 2 diabetes, your daily...
Read more

June is Pride Month, which means it’s time for gathering, festivities, showing up as our...
Read more

Do alcohol and diabetes mix? If you’re a newly diagnosed adult living with type 1...
Read more


