These Are All The Hormones That Diabetes Impacts
Written by: Christine Fallabel
7 minute read
November 25, 2025
Insulin—a hormone produced in the pancreas that allows the body to convert food into fuel—is a hormone without which humans cannot survive. People living with type 1 diabetes no longer make the hormone, so must inject or use an insulin pump to receive it, making life-impacting dosing decisions 24/7. But did you know that there are other hormones people living with type 1 diabetes either don’t make, don’t make enough of, or cannot regulate correctly? While insulin is the life-sustaining key, these hormones have significant effects on the body too.
Glucagon
People with type 1 diabetes have malfunctioning beta cells, so they can no longer produce (or only produce tiny amounts of) insulin. But within the pancreas, alpha cells—which produce glucagon—are also impacted.
In people with fully functioning alpha cells, glucagon releases throughout the day—particularly overnight and between meals—to regulate the body’s glucose and therefore fuel levels. Because the body of a person with type 1 diabetes doesn’t do this in a regulated way on its own, this makes manually balancing insulin and blood sugar levels in the body imperative to survival.
This lack of ability to regulate glucagon secretion also impacts meal time for people with type 1 diabetes. While a non-diabetic’s body would lower glucagon release during and after a meal, allowing the sugar from the food to step in to be the body’s needed fuel source, a person with type 1 diabetes body doesn’t do this, causing the system to get overloaded with both sugar from the food and glucagon, causing blood sugar levels to spike. Additionally, glucagon present in the system signals the liver to make more glucose, causing blood sugar levels to spike even more.
Learn more about glucagon (including the glucagon device options available), and when you should use it.
Incretin Hormones
Alongside glucagon, there are two incretin hormones—metabolic hormones that stimulate a decrease in blood glucose levels—that are not accurately regulated in people with type 1 diabetes.
GLP-1 (glucagon-like peptide) and GIP (glucose-dependent insulinotropic polypeptide) act as the traffic directors for insulin and glucagon—when eating, they would typically signal beta cells to increase insulin production and signal alpha cells to decrease glucagon production. In the absence of functioning insulin-producing beta cells and without these traffic directors working properly, blood sugar management around mealtime becomes difficult.
Additionally, GLP-1 also works to slow down how quickly food empties the stomach. For people with type 1 diabetes, this process isn’t regulated properly, leading to issues with satiety, or appropriate feelings of fullness after a meal. Lack of GLP-1 regulation may also contribute to some stomach-emptying problems such as gastroparesis, a condition in which the stomach cannot empty itself of food in a normal way, which some people with diabetes experience.
There are some GLP-1 drugs on the market. They are approved for use in type 2 diabetes but some doctors may prescribe their use for people with type 1 diabetes. You can learn more about them here.
Amylin
In a person with type 1 diabetes, beta cells—which create insulin—no longer function. Insulin is the most obvious hormone to replace manually, as without it we die. However, beta cells are also responsible for producing another important hormone called amylin. Without functioning beta cells, people with type 1 diabetes cannot make amylin either.
Amylin works similarly to GLP-1. When present in the body, it slows down the rate at which food empties the stomach into the small intestine and helps suppress alpha cells from releasing glucagon; both actions keep blood sugar levels from increasing too sharply after eating or drinking.
Glucagon also signals the body’s appetite, so when amylin and GLP-1 are working correctly to suppress glucagon secretion when and after eating, your brain and body knows that it does not need to keep consuming food. A person with type 1 diabetes may find that they don’t feel full or satiated after what should be an adequate amount of food, or fuel, for their body’s needs.
In other words, if you feel hungry all the time, it’s not your fault. This is another thing to blame on your malfunctioning beta cells.
An amylin analog (a drug with the generic name pramlintide) is available as an injection and works similarly to GLP-1 drugs, but is approved for the use in type 1 diabetes. If you struggle with post-meal blood sugar control or weight gain due to constant appetite issues, one or the other may work well for you.
Adrenaline, Cortisol and Growth Hormone
Known as stress hormones, adrenaline (also called epinephrine), cortisol and growth hormone (also known as human growth hormone, or HGH) each make blood sugar levels rise when released. When regulating correctly, they are vital to human survival. They help the body focus on the task at hand, sometimes shutting off non-essential functions in the immune, reproductive and growth systems to focus on an emergency, while increasing the brain’s use of glucose, tissues’ ability to repair themselves and helping to regulate mood and fear. But when overstimulated, either due to external stress or internal stress caused by blood sugar swings or other health issues, they can each begin causing problems, particularly impacting blood sugar levels and hormone regulation in people with diabetes.
In people who experience low blood sugar, adrenaline is a hormone released by nerve endings and the adrenals to help signal to the brain that something is wrong, and to help the body recover from hypoglycemia (low blood sugar).
For people who experience low blood sugar often, the nervous system can become desensitized, leading to a lack of adrenaline secretion, then causing low unawareness. Luckily this can be treated by going low less often, allowing the body to readjust to normal blood sugar levels and reestablishing an appropriate adrenaline response to signal a low. On the flip side, adrenaline can also adversely affect your body’s health when activated due to being overly stressed.
Cortisol aligns closely with the effects of adrenaline in people with type 1 diabetes. Meant to help regulate the activity of insulin in the body and aid the body with extra fuel through a stressful situation, cortisol is a steroid hormone secreted in the adrenals. But when overactive, cortisol can make a body resistant to the effects of the insulin it requires. In a body that can regulate its own blood sugar levels, this can be okay. But in a body where blood sugar levels must be manually managed, cortisol release means high blood sugar levels.
Like cortisol, growth hormone counterbalances the impact of insulin on muscle and fat cells. The hormone is vital to healthy bodily function, regulating metabolism and energy levels, but can also be overactive in people who experience low blood sugar, as the body will sometimes release growth hormone to help respond to a low.
While stress hormones are necessary for treating low blood sugar levels to help the body react, when you start with stable blood sugar levels and experience stress, it may have the opposite effect on the body. This further reinforces the importance of stress management and nurturing the mental health of patients with type 1 diabetes.
Awareness and a knowledge and understanding of how hormones in the body are affected in people with type 1 diabetes may help to prevent complications, address onset issues and improve overall blood sugar management and control.
Becoming aware of how your body works as a person with type 1 diabetes may help you feel more empowered and capable of handling the woes that come your way. While type 1 diabetes undoubtedly has many difficult days, if this science has any introspective takeaway, it’s that people with type 1 diabetes are a lot stronger and resilient than we know—than you may know of yourself.
Related Resources

While living with type 2 diabetes, getting standard diabetes supplies and medications like insulin, blood...
Read more
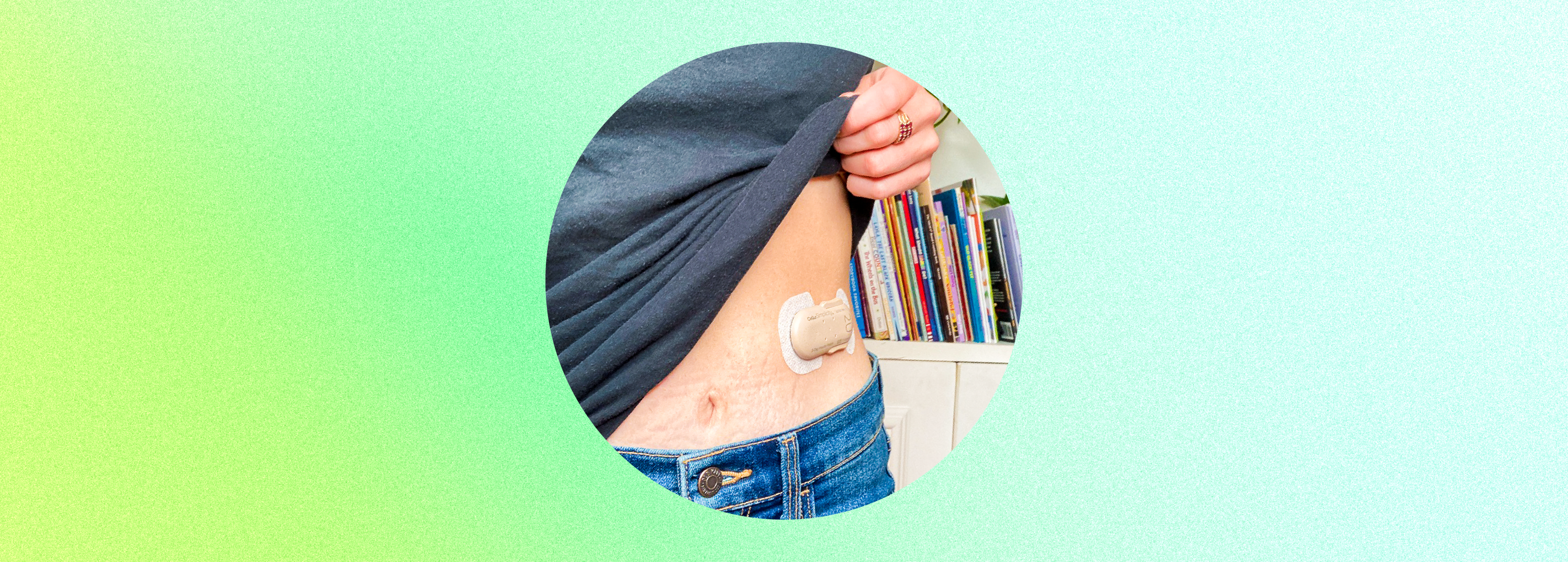
Editor’s Note: Educational content related to insulin patch technology is made possible with support from...
Read more

Attorney, copywriter and Beyond Type 2 community member, Alex Charnin, shares her personal journey of...
Read more


