Severe Hypoglycemia at 31,000 Feet
Written by: Mariana Gómez
8 minute read
March 1, 2026
Editor’s note: This article discusses severe hypoglycemia and does not substitute for medical advice from your health care team. Severe low blood sugars—in which you are unable to eat or drink food, are vomiting for any reason, or overdosed on insulin—may require emergency glucagon and/or emergency services by calling 911.
I boarded my plane at 11:55 pm on my way to the 2022 ADCES conference. In 2006, I completed my first diploma as a diabetes educator, and I have lived with type 1 diabetes since 1984, so I certainly consider myself a specialist.
Using technology to manage my diabetes has given me many privileges. The technology I use helps me make decisions in real-time, so I need some reminders and alarms on my insulin pump and continuous glucose monitor (CGM). Traveling by plane at night with alarms is not the best if you want to go unnoticed. Thinking about not bothering my seat neighbors, I decided to put my alarms on silent.
My blood glucose dropped for some reason during the flight. It dropped so low that my seat neighbor kindly woke me up to ask if I was okay as I was drenched in sweat. I thanked her for the gesture and treated my low blood sugar with her help and the help of another passenger. I experienced a severe hypoglycemic episode on a plane—alone, far from home and explaining what was happening in another language.
My automated insulin delivery system (AIDs) acted quickly to save my life and suspended insulin dosing. By the time I got off the plane, I had already spent more than four hours without any active insulin in my body.
I knew something was seriously wrong
I got off the plane feeling physically horrible, but somehow I felt even worse that I had possibly made my seatmates uncomfortable—I was so embarrassed. I managed to pick up my luggage and head for my hotel. I got to my room, but I don’t remember how or when.
From one second to the next, a very intense pain in my chest made me feel like I had to sit on the floor. I was having a lot of trouble breathing and my left arm was totally numb. I know a little about heart health, and to me, this feeling was a major warning sign of something serious.
I called my colleague, T’ara, and explained what was going on. I told her I would call 911 and she would find my bedroom door open. Still, I kept thinking, “How embarrassing!”
She arrived before emergency services. I repeatedly told her, “I’m so sorry.”
She quickly called 911 again to expedite the process. Within minutes, the paramedics came in and asked a series of questions.
Being blamed for a diabetes emergency
When asked if I was taking any medications, I answered, “Yes, insulin. I live with type 1 diabetes.”
“Ahhh, you have diabetes,” replied one of them, seeming to normalize the gravity of this experience.
“When was the last time you checked your blood sugar levels?” he asked me with a tone of laziness, seeming to assume that I had probably not done it for months.
“My blood glucose at the moment is over 16.6 mmol/L300 mg/dL. That’s not usual for me, and I feel very bad,” I said, explaining my symptoms to him yet again.
“It’s important to take care of your diabetes,” he told me in a condescending manner. “These are things you can do on your own. You don’t need help from anyone. You have to take care of your glucose.”
He blamed me for my situation. Then, another emergency responder became aggravated with me, too, and explained, “It’s important that you use your insulin as well.”
When medical professionals don’t understand diabetes—but refuse to listen
I told him that my blood glucose would continue to rise and the pain would surely cause it to rise a little more. Now becoming even more annoyed, he proceeded to give me a 30-second lecture on how that was not possible, that pain does not cause high blood sugars and that what does cause high blood sugars is improper management.
I first tried to discuss counter-regulatory hormones with him, but this was a losing battle and I was feeling worse by the second.
I was taken by ambulance to the nearest hospital and all I could think was, “My god, how much is this going to cost me? I’m not going to be able to pay for it—this is embarrassing.”
No one should be thinking that when their life is danger. Embarrassment should be your last concern, especially when—despite good management—diabetes can still be out of your control.
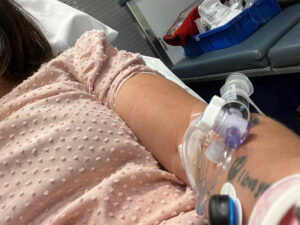
The last thing I needed: advocating for myself in an emergency
In the ambulance, they hooked me up to a myriad of things. I noticed that my hand looked very dehydrated, so I thought, “This is diabetic ketoacidosis.” Also known as DKA. I asked them to check my blood glucose level, and they told me that had nothing to do with it—that they didn’t know what it was.
I arrived at the hospital and repeated the same request. I was told it could not be ketoacidosis because I was on an insulin pump. The doctor—who was actually very kind—told me he had never seen ketoacidosis in a person with type 1 diabetes on an insulin pump.
I was taken to a room where I was given an IV. My blood glucose was now over 22 mmol/L400 mg/dL, and I had no access to my phone or insulin pen. When I asked for it, I was told that they would dose insulin to lower my blood glucose very quickly and that I would feel great soon.
His evaluation didn’t add up to me. Yes, I need insulin but I am extremely sensitive to insulin—and he isn’t discussing my normal insulin doses or sensitivity with me at all. Additionally, I know my body also needs other levels checked. During DKA, insulin is usually administered along with electrolytes and other critical ingredients to balance everything, not just your blood sugar. Not taking this step can lead to other serious issues.
How diabetic ketoacidosis should be treated
In my experience as a specialist myself, I knew that a timely diagnosis, comprehensive clinical and biochemical evaluation and effective management are key to the successful resolution of DKA.
Critical components of hyperglycemic crisis management include:
- Coordinating fluid resuscitation
- Insulin therapy
- Electrolyte replacement
- Continuous patient monitoring using available laboratory tools to safely and accurately predict the resolution of the hyperglycemic crisis
- Understanding and prompt awareness of potential special situations such as DKA or hyperosmolar hyperglycaemic syndrome (HHS) presentation in the comatose state
- Possibility of mixed acid-base disorders obscuring the diagnosis of DKA
- Risk of brain edema during therapy
These are all critical touch-points doctors treating people with diabetes, like myself, need to evaluate to help reduce the risks of complications without affecting the recovery from a hyperglycemic crisis.
This was not the process I was seeing at the hospital, so I insisted they test for ketones. That didn’t happen. Instead, they continued to insist that they would quickly correct my blood glucose with a lot of insulin.
“You’re not a doctor,” a nurse explained. “The doctor will decide what kind of insulin and the quantity you’ll need.”
My life was in danger.
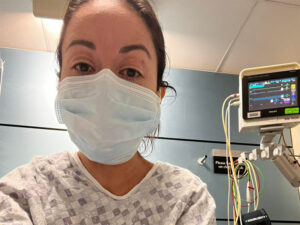
I told myself, “Do not lose consciousness.”
My mission now consisted of three things:
- Stay conscious.
- Measure ketones.
- Reach into my bag to keep track of my insulin and data.
They weren’t listening. They were always kind, but they didn’t seem to trust that I had any idea about what was going on.
“I’m not having a heart attack—it’s diabetic ketoacidosis, and I need to take insulin,” I insisted.
I managed to get to my bag and was able to start correcting myself before they did. They hooked up the serum, which was clearly not glucose, and I took over my continuous glucose meter. They were still measuring my glucose capillary.
“And what brings you to this city? ” someone asked to which I replied, “I came to the 2022 ADCES conference. I am a diabetes educator.” To which that person replied, “Ha, how ironic.”
Putting my care in my own hands
When my blood glucose finally reached 11.11 mmol/L200 mg/dL thanks to dosing insulin via my pump, I decided to leave. T’ara picked me up, and even though I was feeling horrible, I decided to attend the conference.
While all of that was going on with me, there was a convention center full of diabetes experts, talking about how to create diabetes education programs, the latest in technology and medication, how consultations and practices should be patient-centered and about the art of motivational speaking.
It was all presented by diabetes educators for diabetes educators—in the same city, place and time where the exact opposite was happening to a diabetes educator living with type 1 diabetes. Isn’t that ironic?

What needs to change in emergency medical care
What needs to change in emergency medical care is not blame, but systems. Emergency teams need clearer protocols for diabetes-related emergencies and stronger training on conditions like severe hypoglycemia and DKA. But more than anything, they need to listen to patients who know their own bodies. Care should be personalized and compassionate, not rushed or dismissive. Decisions should be made with patients—not over them. No one should have to explain, defend, or manage their own care while their life is at risk.
References:
Correlation between Peripheral White Blood Cell Counts and Hyperglycemic Emergencies https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3638300/
Author
Mariana Gómez
Mariana is a psychologist and diabetes educator. She is the creator of Dulcesitosparami, one of the first online spaces for people with type 1 diabetes in Mexico. Mariana is currently the VP of International Markets at Beyond Type 1. She was diagnosed with type 1 diabetes more than 30 years ago and is the mother of a teenager.
Related Resources

As you get older, your body and mind change, and that affects how you feel...
Read more

It’s fair to assume that a 911 call about severe low blood sugar (hypoglycemia) will...
Read more
Low blood sugar can make people with diabetes (PWD) feel exhausted, frustrated and scared. Sometimes,...
Read more

