The Magic of Diabetes Camp
Written by: Shelley Yeager, MA, LCSW
4 minute read
July 21, 2016
"Diabetes camp is like a diabetes vacation. It makes me feel like I don't have diabetes because everyone understands. I don't have to explain everything, remember everything, or make decisions all the time. There's always someone to help me."
Campfires, bug juice, epic gaga, best friends—these are the ingredients that stir up summer camp success. Whether your favorite is in the mountains, on the beach, at a college campus or in a city park, summer camp has enriched the lives of youth since 1861. The camp bubble will never be burst. Inside there’s a magic mixture of risk and safety; friendship and respect; laughter and tears; self-awareness and confidence. The “real world” will never threaten the magic of camp.
For youth with diabetes, the choice isn’t whether to go to camp, because every young person with diabetes should go to camp. It’s whether to go to diabetes camp or non-diabetes camp and when to start going. Day camps are a good transition for young children. Overnight weekend, week, month or all summer programs are options for older youth. The choice should be a carefully made family decision. The time is right when it feels right for each individual child and their family. Typically, overnight camps start accepting youth at about age 8, but your child might not be ready until much later. There are many factors that influence this decision. If you are uncertain, talk with the professionals in your child’s life —their pediatrician, teacher, or school counselor. Most importantly, talk with your child. Parental urging is always acceptable but forced attendance may set your family up for a bad outcome.
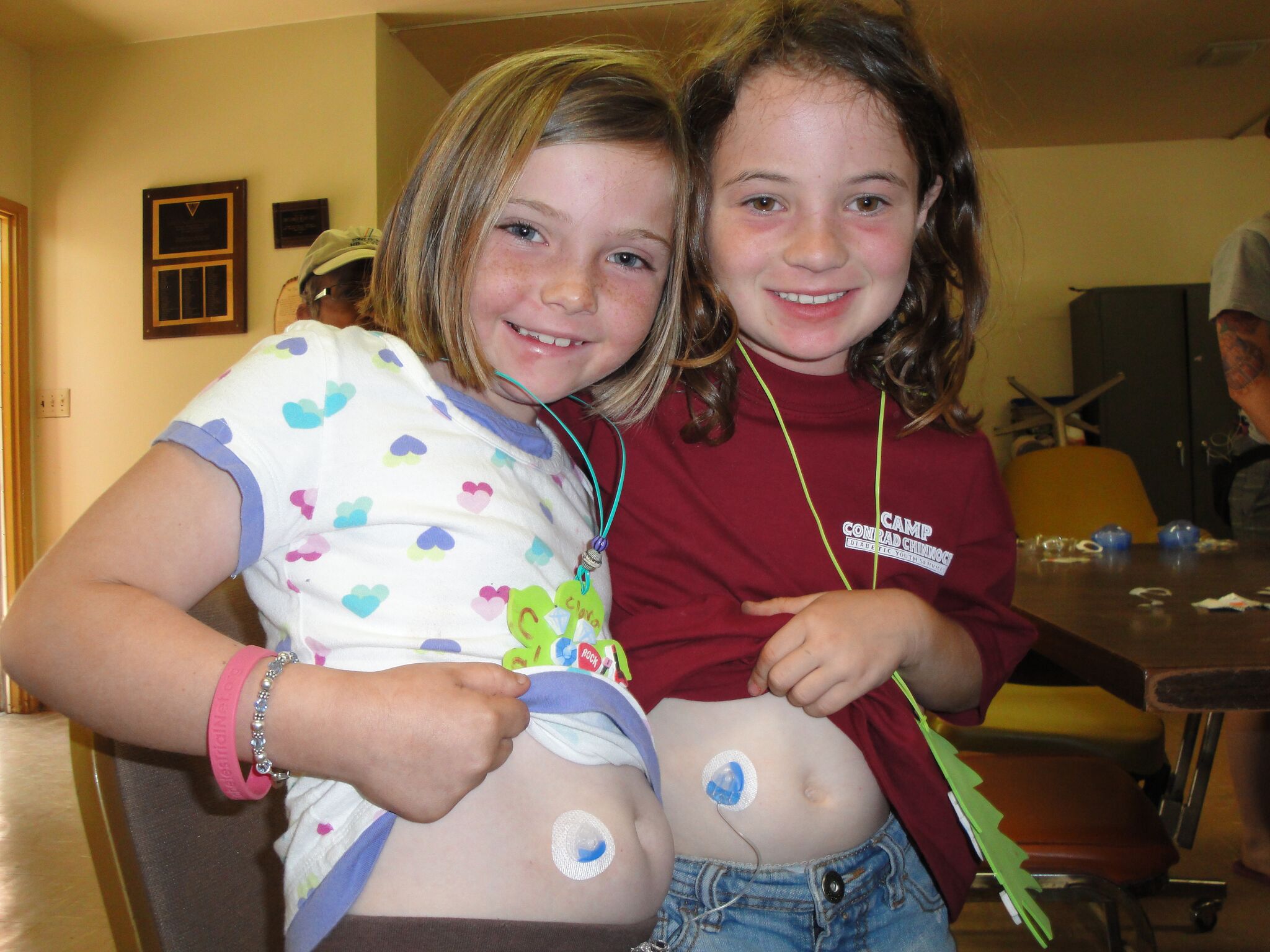
Let’s be clear with the “diabetes” difference. Camps come in all shapes and sizes —day and resident; sports and arts; trip and wilderness; and more. Diabetes camps and non-diabetes camps are similarly diverse. The key difference is that, in a diabetes camp, the key participants have diabetes and the program is developed around their needs. Diabetes camps may be “bring a sibling or friend” or “bring your family.” Still, the program is built around the key participant—the youth with diabetes. In a non-diabetes camp, the program is created around the camp mission itself and, while they may accept the child with diabetes, and safely care for the child, the essence is very different.
I lived, literally, at diabetes camp for 20 years and one of the things that most impressed me was when campers said, “Diabetes camp is like a vacation from diabetes. It makes me feel like I don’t have diabetes because everyone understands. I don’t have to explain everything, or remember everything or make decisions all the time. There’s always someone to help me.” The beauty of diabetes camp is that you get the wonderful elements of camp—motivation, risk taking, learning new things, friends—wrapped into a place where everyone understands diabetes and is equipped every minute to deal with the diabetes moment such as a low, a high, a pump site dislodged, a bolus calculation, a sick day. A camper with diabetes is never alone without another diabetes expert to help—a role-model counselor, a nurse, a doctor, a friend. It’s hard to measure the comfort of that—and the comfort for parents knowing their child has the most competent care. At a JDRF presentation I did the other night a parent said, “When I dropped my 8-year-old off at camp last summer, I just knew she was in expert hands. They asked all the right questions. I feel great about sending her for two weeks this summer.”
Yet, there are other choices. Maybe there is a camp that your entire family attended or a specific sports or arts camp that interests your child. Non-diabetes camps are increasingly able to handle diabetes. Many will attest to the fact that they have a nurse or nurses on site who understand diabetes (and pumps). Many are school nurses who have students with diabetes during the school year. And, if a parent is really lucky, the camp may have staff members who have diabetes. The key to sending your child with diabetes to a non-diabetes camp is to do your homework.
Consider the following…
- What is the ratio of nurses to campers?
- Who will be trained and equipped to handle your child’s diabetes when they are not in the health center?
- How will insulin be adjusted and administered?
- Who will treat lows?
- Where will low supplies be kept?
- Is the menu “friendly” for your child, can you see it in advance to discuss options with your child before they go?
- Does the camp have a procedure for diabetes management at the waterfront, on trips out of camp and at high risk activities?
- How much pressure will be on your child for self-management decisions without adult intervention?
- At day camps that provide transportation, is there someone on the bus equipped to deal with an urgent diabetes need?
- How does the camp handle transitioning the child from home to camp?
- What were blood glucose values overnight and how does that play into today’s activities?
- Does the camp know to care?
- Are you on board with the answers?
Doing your homework will make this option a great one and will preserve that “camp magic” forever. In closing, don’t forget to take your prospective camper to visit at “Open House” day. Most camps, whether day or resident, have them. Meet the staff and other campers—get the “feel” of it. You’ll know when it’s right.
Whichever you choose, at the end of the summer it will be campfires, bug juice, epic gaga and best friends that you’ll be hearing about…and, of course, camp songs at the dinner table. Happy camping.
For more information
- For all diabetes camps: Diabetes Education and Camping Association’s website.
- For ADA camps only
- Non-diabetes camps and camp accreditation
- General Camp FAQs
Read Why I Love Diabetes Camp from Kip Nilsson, aged 9.

Author
Shelley Yeager, MA, LCSW
Shelley Yeager, MA, LCSW, is the program & development specialist at the Diabetes Education & Camping Association. She does consultations with diabetes youth programs and can be contacted at [email protected].
Related Resources

Antoine Gibson is no stranger to overcoming challenges. As a saxophonist and marathon runner living...
Read more

Danica Collins not only prepared for one of the most challenging physical events of her...
Read more

Beyond Type 1 is spotlighting inspiring athletes with type 1 diabetes as they prepare for...
Read more

